Posted on by davidhencke
Last year I reported on the tragic death of talented 25 year old Gaia Young 17 hours after she was admitted to University College Hospital with severe headaches. Her mother Lady Dorit Young was subject to an entirely unsatisfactory and unsympathetic coroner’s inquest by Mary Hassell which let the hospital off the hook saying the cause of death was unknown. You can read my original blog here.
The coroner blocked Lady’s Young’s attempt to get independent evidence from a neurologist but since then she has managed to get an independent neuro-radiologist and neurologist’s report and UCLH have opened a further review into her tragic death.
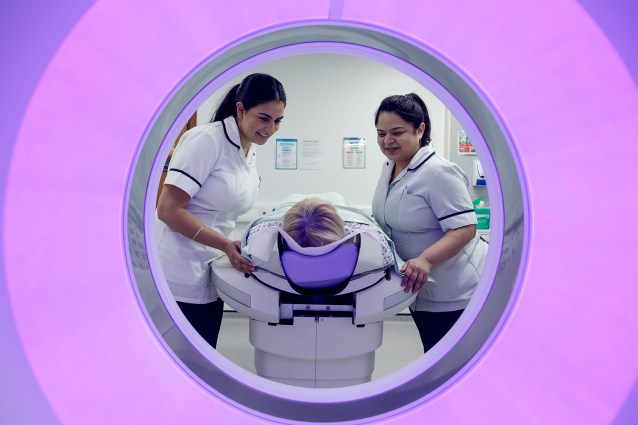
The protest vigil on September 15 was sparked by the findings of the neuro radiologist who examined the CT scans of Gaia’s brain. It showed quite clearly even to a lay person, according to Dorit ,that the first scan taken and I quote ” there is a gross cerebral and cerebellar swelling. There is effacement meaning ( ” literally meaning ‘ rubbed out’: these fluid spaces should be visible but cannot be seen).”
This is the opposite to the consultant radiologist who examined Gaia’s scan who said: “The ventricles and basal cisterns are patent…Impression No acute intracranial finding.”
The independent consultant’s diagnosis was confirmed by Dr Charles House, the medical director, when he met Dorit and compared Gaia’s scan with a normal brain scan.
The consultant radiologist who examined this first scan was Dr Ayman Mahfouz, who was on duty at UCLH at the time Gaia was admitted. Dr Mahfouz, has a private practice in Harley Street.
His entry on the private practice site says he has specialist expertise in breast, gynaecology and general imaging.
He undertakes all aspects of breast imaging including mammographic (plain, contrast enhanced and 3D), Ultrasound, MRI and CT diagnostics. He performs all ultrasound and stereotactic breast related procedures including vacuum excision.
Dr. Ayman Mahfouz is a designated appraiser for doctors at UCLH and has previously been elected as a regional representative for doctors in training at the Royal College of Radiologists. At the time of Gaia’s admission he held the role as Emergency Imaging Lead for UCLH.
Gaia’s mother would like to contact him about the scans but so far he has not responded. She does not know what pressure he might have been under at the time or how much time he took to examine the scan. I did ask UCLH about whether he wanted to say anything about this but there was no response to my question.
UCLH did issue a response about the review into Gaia’s death.
A UCLH spokesperson said:
“We met with Lady Young and apologised that Gaia’s care fell below the high standards we strive to provide. We sympathise greatly that the cause of her beloved daughter’s death four years ago is still unknown.
“We are committed to learning from external opinion and scrutiny and have commissioned a range of independent experts to explore further the circumstances surrounding Gaia’s death. We agreed with Lady Young the scope of the reviews and the experts who will undertake them.
“We await the outcomes of all the external reviews to understand if further lessons can be learned and acted upon.”
Dorit’s vigil last month caused more than a flutter on Harley Street. The clinic at 99 Harley Street called the police and also alerted its own security guards. When the one man patrol car turned up with flashing blue lights the policeman turned out to be incredibly polite and said no-one was breaking the law so long as the entrance to the premises and pavement was not blocked.

Then two security guards turned up, saying they had been informed by a member of the public that large numbers of people were demonstrating there. It turned out to be just three people and they were remarkably friendly and polite when they heard about the circumstances. They didn’t mind having their pictures taken.
The one person who didn’t turn up was the doctor and one of his private practice colleagues politely remonstrated with us that this was not the right way to do things and Dorit should arrange a meeting with the hospital. It was pointed out to him she had been reprimanded by the Trust on various occasions for trying to contact clinicians having cared for Gaia. She never received an answer. The Trust never offered a meeting with any of these doctors.
Gaia’s case has been taken up by an Islington councillor, Dr Hannah McHugh. She wrote a strongly worded opinion piece for her local paper, The Islington Tribune. You can read it here.
She says:” As an Islington councillor, I’ve supported Lady Young in this painful journey. It has revealed something of concern to us all: when things go wrong in our healthcare system, the path to truth is too often long, difficult, and unjust. Tragedies become injustices.”
Slowly but surely the facts about Gaia’s death are coming to light. But so far it has taken four years to achieve with no help from coroner Mary Hassell.
This to me is a general problem across the NHS. Rather than acknowledge to patient’s relatives that mistakes have been made, trust managers initially go on the defensive and are prone to cover up what went wrong and who was responsible. It is only people with guts and determination like Dorit who are prepared to fight for years until they get answers that the true facts start to come to light.
UPDATE; The ex coroner and Lady Dorit Young held a second vigil at a conference organised by the Royal College of Radiologists in London this month to bring it home to the profession the need for the very careful reading of scans by radiologists. Here is a picture of their vigil accompanied by a police officer.

Make a one-time donation
Make a monthly donation
Make a yearly donation
Choose an amount
Or enter a custom amount
Your contribution is appreciated.
Your contribution is appreciated.
Your contribution is appreciated.
DonateDonate monthlyDonate yearlyGaia Young