Former consultant also says old X ray machines at Epsom Hospital put staff and patients at risk from radiation when they are fitted with pacemakers
Dr Richard Bogle, the former head of the cardiology department at the Epsom and St Helier University health trust, admitted to an employment tribunal that the trust should have reported the death of a 76 year old heart patient to the Coroner and the Care Quality Commission three years ago.
The doctor under cross examination from barrister Matt Jackson described the death as “tragic ” and admitted the trust should have informed both the coroner and the CQC. He said that although he was on ward duty he did not know anything about the patient and ” couldn’t have been expected to know about all the patients at St Helier hospital.”
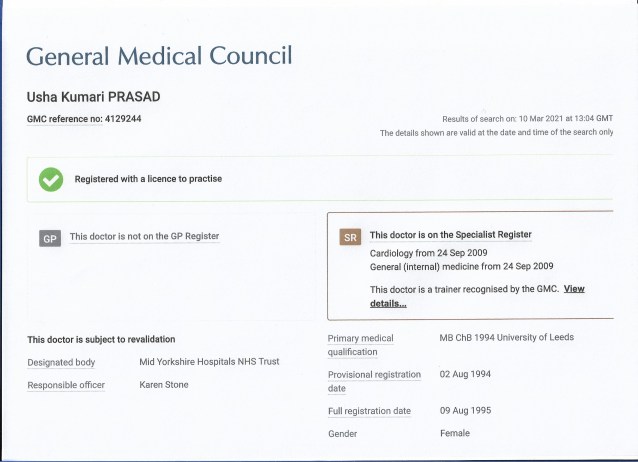
The details came out at a recent tribunal hearing under Judge Anthony Hyams-Parish, brought by Dr Usha Prasad, a cardiologist who has been dismissed by the trust even though the General Medical Council has exonerated and re-validated her as “fit to practice” medicine. She decided to make two protected disclosures under the Whistleblowers Act after the trust covered up her findings on the death. You can read a series of previous articles on this blog about the battle Dr Prasad has had with senior staff at the trust.
The disturbing case of patient Mr P
The patient known as Mr P was admitted in August 2018.Dr Prasad’s witness statement said :”He died of heart failure on 5 September 2018 having been previously admitted from 5 to 15 of August to Ward 6 which is a ward run by cardiology and respiratory medicine at St Helier hospital. Mr P had been admitted with breathlessness and diagnosed with pneumonia. However, an echocardiogram had been ordered by Dr Foran (Cardiologist) which showed evidence of “severely impaired left ventricular systolic function…. [with a] drop in left ventricular function since last scan, previously mildly impaired.” The echocardiogram was performed when Dr Richard Bogle was assigned to the ward and the results could not have been known by Dr Foran. The pneumonia was successfully treated by the respiratory physicians and Mr P was discharged after about 10 days. The echocardiogram had shown signs of severe left ventricular failure but the results were not recognised by the chest physicians or cardiologists on the ward. The patient was discharged after having largely recovered from the pneumonia during his first admission and then was readmitted on 4 September with severe left ventricular failure from which he died shortly afterwards on 5 September 2018. The certified cause of death was heart failure.”

Dr Prasad was assigned by Dr James Marsh, the medical director to write up a report on the patient’s death. Her conclusion was that it was a Serious Untoward Incident Level 5 – that is the hospital caused severe harm to the patient leading to his death. This would lead to a report to the coroner and the CQC. The coroner could look at how the patient died and the issues surrounding it to help prevent other deaths.
What followed were attempts by other senior consultants to water down the report and delay its completion which Dr Prasad refused to do. Those involved in this exercise included Mr Karim Bunting, the quality manager at the trust and Dr Simon Winn, Clinical Director for Acute and General Medicine, She was asked to make the report in her words “inaccurate” and Dr Winn drafted an alternative version. He accepted that a serious mistake had been made by not recognising the result of the echocardiogram but put the emphasis on the lack of communication between the respiratory physicians and the cardiologists. He did not accept it as an avoidable death.
It is not known whether the patient’s relatives were properly informed about the circumstances of the death or which version of the report they have been shown if any. There is a duty of candour if someone has died.

The second disclosure of failings at the hospital that came out at the tribunal concerns serious radiation risks from old X Ray machines at Epsom Hospital – which are used when pacemakers are inserted into patients. This puts staff and patients at risk.
Dr Sola Odemuyiwa, consultant cardiologist at Epsom Hospital from 1994 until 2016, He disclosed how an audit by Dr Abhay Bajpai, – specialist in pacemaker devices and electrical rhythms, appointed to take over pacing at Epsom in addition to his other duties – revealed stark contrasts in radiation levels between Epsom and St George’s hospitals. Using a dosimeter, he compared radiation insertion of a similar number of devices at St George’s. With similar average screening times, the total radiation received was substantially higher (up to a hundred times greater) at Epsom than at St George’s.
He says in his witness statement: “When I saw the histograms – the Micrograys of radiation from Epsom a skyscraper beside which the values from St George’s, looked slipper thin, (I attach the relevant data) my heart drummed against my ribs out of apprehension and angry self-reproach as I recalled with dismay how for twenty years I may have been gorging my organs on X-rays. My anxieties ballooned when I learned that Abhay’s readings came from Libra, the more modern of the two machines and that I was often given the older Endura machine, which emitted even higher levels of radiation.”
“Drs Yousef Daryani and Abhay Bajpai, my colleagues on the Epsom site continued to press the Trust over the safety of the X-ray machines. In February 2016, Abhay presented his audit data again at a meeting between Cardiology and Radiology departments. He thought the machines should be replaced. The senior radiographer said she could not change the past but that the machines were working properly.”
He then sought figures for radiation doses he had received during his career at Epsom Hospital.. “The Radiation Protection department at George’s were most helpful and sent me dose records from 2005 to 2008. Where are the data from 1995 I asked. They said they could not retrieve the data from the archive of the Mirion Technologies Dosimetry Services Division.”
The trust itself is adamant that there is nothing wrong with the machines. A long e-mail trail between the consultant and trust officials ended with the Trust insisting that the machines are safe and regularly checked.
Sally Lewis ” our image intensifiers are old and due for replacement “
Sally Lewis, a radiologist and medical examiner at the trust, wrote to Daniel Elkeles, then chief executive of the trust, saying there had been confusion about the reporting of the differing level of doses at Epsom and St George’s using different methods. She said if they had exceeded safety levels it would have triggered an alert.
She admitted; ” We are well aware that our image intensifiers are old and due for replacement … newer machines will with new technology produce lower dose readings which is something we always strive for.”
Dr Odemuyiwa disputes her findings. He said: “The manager misunderstood the report from the Radiation Protection Service. The absorbed dose of radiation, the amount of energy deposit in a small volume of tissue, and the equivalent dose, the impact that dose has on that tissue are numerically the same. The former is measured in mGy and the latter in mSv or milliSievert. Colon and prostate are more sensitive than the head for example.”
A year after leaving the trust he was diagnosed with prostrate and bowel cancer.
He explained to me in an interview: ” When you are fitting a pacemaker you are lying over the patient and are very close to the imaging equipment. If you are going to receive too much radiation the most sensitive organs to cancer are the prostrate and the bowel.”
Dr Odemuyiwa: ” When you are fitting a pacemaker you… are very close to the imaging equipment”
Since he announced his support for his colleague, Dr Prasad, Epsom and St Helier University Trust have declined to revalidate him so he cannot practice medicine.
The trust were contacted about what they intend to do after these revelations but have not responded.
Epsom and St Helier University Trust say on their pinned tweet on Twitter: “We put the patient first by giving outstanding care to every patient, every day.” Draw your own conclusion.
A second blog will look at what the hearing revealed about the issues surrounding the treatment of Dr Usha Prasad. The tribunal is expected to issue its findings in the New Year.
Please donate to my blog Westminster Confidential to help me continue my forensic work.
Make a one-time donation
Make a monthly donation
Make a yearly donation
Choose an amount
Or enter a custom amount
Your contribution is appreciated.
Your contribution is appreciated.
Your contribution is appreciated.
DonateDonate monthlyDonate yearlyPlease donate to Westminster Confidential
£10.00